- In the 1950s, Europe was recovering from a devastating war. Food policies were devoted to establishing secure, adequate supplies of food for the population. Refugees and food rationing were still huge problems, and the European Region relied heavily on countries such as Australia, Canada and the United States to provide its bread, cheese and meat. By the mid-1970s, strong national and regional measures to support agriculture had helped ensure better agricultural supplies within the WHO European Region, in both the western and eastern countries. In general, there was plenty to eat, and a huge food processing industry had become well established. Yet all was not well. By the 1980s, policies in western Europe had been too successful, creating problems of overproduction and what to do with the huge amounts of food that were not being eaten. In eastern Europe, the political changes of the late 1980s and early 1990s led to increasing problems with food supply and distribution. In addition, the movement of food increased in the 1990s, in terms of both the quantity transported and the distances travelled. Across the Region, there was evidence of increasing rates of disease related to the food being eaten: rising rates of foodborne infectious disease, rising rates of deficiency diseases in pockets of the Region and high rates of chronic, degenerative diseases in which diet plays a key role. The impact of these diseases – the burden on health services and the costs to economies, societies and families – is beginning to be seen. In particular, health services are becoming conscious of the share of their budgets consumed by food-related ill health. In response, health policy-makers are turning their attention upstream, looking at the early causes of ill health, rather than its diagnosis and treatment. This enables policy-makers to explore possibilities for reducing the burden of disease on the health services and improving the health of the population at large. This book supports these health policy initiatives. It reviews the current burden of food-related disease in the European Region, examines the links between disease and food, and looks upstream at the nature of food supplies. It 2 Food and health in Europe shows that policies on food supply and a range of related topics – such as sustainable agriculture and rural development, transport and food retailing and planning – are all linked to the problems of nutrition, food safety and food quality. In doing this, the book recognizes the very uneven patterns of food production, food safety problems and diet currently prevailing in the European Region. These patterns vary widely between the Nordic, central and Mediterranean countries in the European Union (EU), and even more among the countries of central and eastern Europe (CCEE) and the newly independent states (NIS) of the former USSR. In addition, agricultural policies and support measures differ; food distribution and consumption patterns differ; dietary disease incidence and prevalence differ. These differences can help to reveal the causes of ill health, and point towards their solution. This book gives data where the figures are available, and points to areas where they are lacking.1 It shows that knowledge about the links between food production, distribution and consumption and subsequent health patterns is now sufficient to enable these elements to be seen as parts of a greater whole. This whole is influenced by past and present food policies, and can influence future policy-making. Overview of the book This book lays out the available data that show the links between health, nutrition, food and food supplies, as outlined in the First Action Plan for Food and Nutrition Policy, WHO European Region, 2000–2005 (Annex 1). Rising concern about health and consumer issues has led EU countries explicitly to include assessments of the effects on health of other sectors’ policies, in accordance with the Amsterdam Treaty. The Action Plan recommends that WHO Member States within and outside the EU develop cross-sectoral mechanisms to ensure that health policies are integral to non-health sectors. The WHO Regional Office for Europe has expressed its commitment to supporting Member States in this task. Diet and disease Care needs to be taken to distinguish the share of disease attributable to poor diets and that avoidable through better diets. Two assumptions underpin the analysis of the costs and burdens of diet-related ill health: that diet can be a primary cause of disease or cause a reduction in disease, and that the extent of 1 Food and health in Europe: a new basis for action. Summary (http://www.euro.who.int/InformationSources/Publications/Catalogue/20030224_1). Copenhagen, WHO Regional Office for Europe, 2002 (accessed 3 September 2003). Introduction: the need for action on food and nutrition in Europe 3 this causation can be measured. Arriving at agreed figures for the extent of causation is not simple. In many diseases, diet is only one of many contributory factors (such as smoking or lack of physical activity), and even the dietary component may vary in different circumstances. Attempts need to be made to tease out the relationships. Chapter 1 looks at patterns of disease and their links to diet. Fundamental to examining patterns of disease is the notion that they vary between places or over time. These differences allow the suggestion of reasons, which imply causative links, and of remedies, so that people with higher rates of disease may experience the lower rates enjoyed by others. Chapter 1 reviews chronic noninfectious diseases with links to diet, including the major causes of death in the European Region (cardiovascular diseases and cancer) and those that may not kill but nevertheless are costly to health services, such as dental disease and hypertension. The role of physical activity as an independent and complementary factor reducing the risk of dietary diseases is highlighted. Chapter 1 also discusses deficiency diseases, such as those related to iodine and iron deficiency, which are still widespread in parts of Europe, including subpopulations in western European countries, and Chapter 4 considers their implications for food and nutrition policies. Chapter 1 presents nutrition data during key stages in the human life cycle, and considers the possibilities that fetal, infant and childhood nutrition may have long-term implications for chronic diseases in adulthood. Economic status – expressed as household income, earnings or employment category – appears to be a major determinant of many diseases that are known to have dietary links. As illustrated at the end of Chapter 1, poverty is associated with a higher level of risk for these diseases. Various policy implications can be derived from this, and Chapter 4 highlights such issues as access to healthier foods, their cost, the need to store and prepare them, planning and transport policies, education policies and priorities, advertising policies and the social provision of foods through schools and hospitals. Food safety Chapter 2 presents short reviews of the links between food safety, health and foodborne diseases. It also looks at toxicological and food safety issues, and considers concerns about the contamination of food with toxic chemicals (such as dioxins), potent microbial agents (such as Escherichia coli 0157) and bioactive proteins (such as protease-resistant prions), as well as longer-standing concerns about the impact on health of agrochemicals and veterinary drugs used to enhance agricultural productivity. Good evidence links these aspects of food and health – principally food safety and nutrition – in certain circumstances. Each affects the other. On the 4 Food and health in Europe one hand, nutritional status can determine the risk of infectious disease, and dietary patterns can lower the risk of infection. On the other, foodborne disease can reduce nutrient intake. Food security and sustainable development The role of food production in generating food-related ill health forms an integral part of this book. Chapter 3 discusses methods of agriculture and food processing, the types of food produced and the increasingly long distances that food commodities travel. Although production is frequently asserted to follow the patterns of food demanded on the market, there are good reasons to suggest that food production has become dissociated from market demand and that many factors distort the market. The forms of food production determine not only food products’ safety but also their nutritional and dietary value. Food production methods – and the factors that influence them – thus form an integral part of the patterns of food-related ill health. Environmental issues, especially the need to develop farming methods that are sustainable in the long term, have a bearing on food production. A broad degree of concurrence can be foreseen between the production of food for human health and the production of food for environmental protection. Nutrition and environmental policies can thus be developed in parallel, as outlined in the WHO Action Plan. Food production affects human health in other ways than through food consumption. The nature and sustainable development of the rural economy have implications for rural employment, social cohesion and leisure facilities. These in turn foster improved mental and physical health. These issues are not mere by-products of sustainable development; they are central to the retention of rural social structures. The wider costs of conventional intensive agriculture have been described, and Chapter 3 gives some figures on their economic impact. Any health impact assessments of rural environmental policies and agricultural policies need to consider these largely hidden costs of different farming methods. Chapter 3 explores a model of social capital and social dividends, and different food production methods can be shown to help increase or deplete them. Hidden costs or externalities (costs that are not directly borne by the production process) affect both agriculture and food processing, packaging and distribution. Transport, for example, has relatively low direct costs, but can have much higher true costs when externalities are taken into account. These hidden costs include pollution and traffic accidents. They not only indicate that the activity is not sustainable in the long term but also directly affect health, and hence place a burden on society and the health services. Introduction: the need for action on food and nutrition in Europe 5 Policies and strategies Ensuring the safety of food is regulators’ and legislators’ first priority; its health promoting features and its sustainable supply come second. Breaches in food safety can lead to immediate and often fatal outbreaks of food poisoning, and the main thrust of food inspection and control procedures is to ensure that food is safe to be eaten. Changes in food production methods, discussed in Chapter 3, have led to the changes in food control strategies discussed in Chapter 4, such as the adoption of hazard analysis and critical control points (HACCP) procedures. In addition, as discussed earlier, it is useful to look upstream and ask why contaminants and hazards find their way into the food supply, rather than relying on minimizing the risks from those that are already present. Looking upstream at food production is one valuable step, but others also need to be taken. With increasing long-distance distribution of primary and processed products, across national boundaries and around the globe, national regulations are coming under scrutiny, and international agencies (such as the Codex Alimentarius Commission) are increasingly involved in setting safety standards. International standards for the food trade need to be set to protect health, and the health impact of trading policies needs to be assessed. Chapter 4 discusses nutrition policies from the perspective of improving nutrition at key points during the life-course to maximize opportunities for health in later life. The examples given include exclusive breastfeeding in early infancy to prevent ill health in childhood, and the improvement of women’s nutrition before and during pregnancy to ensure optimum growth of the fetus and infant and the prevention of disease in adulthood. Chapter 4 also discusses the setting of population targets for healthy eating. These targets have become increasingly specific in the last 20 years, moving from general statements about the need to eat a healthy diet to numerical recommendations for certain nutrients and foods. Such targets as increasing fruit and vegetable consumption and reducing fat, salt and sugar intake have implications beyond the orbit of health educators and public advice, and are of direct concern to agricultural production and the food processing and retailing industries. Population-based nutrition programmes are required to translate population targets into practice. Such programmes include various measures, ranging from specific initiatives advising on healthy lifestyles to controls over food labelling, health claims and advertising. Messages on healthy eating need to be consistent, and widely accepted and promoted by all stakeholders. Nutrition, food safety and food standards are the policy areas that directly affect food-related ill health. As suggested, many other human activities and the policies that govern them have an influence. These activities include the growing, transport, processing, distribution and marketing of food. Policies 6 Food and health in Europe on these activities can be presumed to have a bearing on subsequent food safety and nutrition, and hence influence health. Health impact assessment of such policies is being developed in various forms across Europe and elsewhere, and the procedures have many common threads. The methods involve iterative processes, so that initial conclusions can be re-examined and refined and additional material added to the analysis. They have the advantage of providing the basis for a democratic form of decision-making, and can increase the transparency of the processes and of the interests involved in policy-making. Different forms of intervention need greater analysis to examine their cost–effectiveness and – efficiency. Surveillance, including monitoring and evaluation, is discussed in Chapter 4. WHO activities Discordant agricultural, industrial and food policies can harm health, the environment and the economy, but harmful effects can be reduced and health can be promoted if all sectors are aware of the policy options. National policies on food and nutrition should address three overlapping areas: nutrition, food safety and a sustainable food supply (food security). The First Action Plan for Food and Nutrition Policy calls for interrelated strategies on all three (See Chapter 4, Fig. 4.1, p. 222). WHO’s traditional roles – supporting the health sector in the provision of services and training of health professionals, advising it on planning and assisting in health programmes – can be extended and developed. The Action Plan outlines a series of support measures for national and regional authorities. This book provides a basis for these actions, founded on scientific evidence on the causes of food-related ill health. 7 1. Diet and disease The burden of disease varies widely within the WHO European Region and has changed dramatically in many countries over the last 20 years. Patterns of disease and changes in these patterns have environmental determinants, with diet and physical activity playing major roles. This chapter assesses the range of major health issues confronting European countries and some of the principal determinants of diseases leading to death and disability. Differences and changes in diet explain much of the different patterns of ill health observed in children and adults. Appropriate public health policies can help prevent the nutrition-related diseases discussed here. Chapter 4 presents recommendations on policy, and cross-references are made where applicable throughout Chapter 1. Diet-related diseases: the principal health burden in Europe The burden of disease has been assessed in terms of disability-adjusted lifeyears (DALYs). These incorporate an assessment of the years of life lost to different diseases before the age of 82.5 years for females and 80 for males (1) and the years spent in a disabled state (2). Non-fatal health states are assigned values (disability weights) for estimating years lost to disability based on surveys. Years lost (severity adjusted) to disability are then added to years lost to premature mortality to yield an integrated unit of health: the DALY; one DALY represents the loss of one year of healthy life. Fig. 1.1 shows the contribution of nutrition to the burden of disease in Europe (3), displaying the share of DALYs lost to diseases that have a substantial dietary basis (such as cardiovascular diseases (CVD) and cancer) separately from that to which dietary factors contribute less substantially but still importantly. In 2000, 136 million years of healthy life were lost; major nutritional risk factors caused the loss of over 56 million and other nutritionrelated factors played a role in the loss of a further 52 million. CVD are the leading cause of death, causing over 4 million deaths per year in Europe. Dietary factors explain much of the differences in these diseases in Europe. The world health report (4) includes an estimate of the quantitative contribution of dietary risk factors such as high blood pressure, serum cholesterol, overweight, 8 Food and health in Europe obesity and a low intake of fruits and vegetables. European policy-makers will need to make their own assessments of the relative burden of dietary risk factors in relation to disease prevalence in their own country. Fig. 1.1. Lost years of healthy life in the European Region, 2000 Source: adapted from The world health report 2000. Health systems: improving performance (3). Diet as a determinant of health The dietary contributions to CVD, cancer, type 2 diabetes mellitus and obesity have many common components, and physical inactivity is also relevant to all four. The overall effect of each dietary component and of physical inactivity should be calculated and their relative quantitative significance estimated. Unfortunately, only one such assessment of the burden of disease attributable to nutrition in Europe has yet been published (5). The National Institute of Public Health in Sweden attempted to estimate the burden of disease that could be attributed to various causal factors, Diabetes mellitus (5%) Malignant neoplasm (32%) Other neoplasms (0.2%) Nutritional deficiencies (2%) CVD (61%) 41% 38% 21% Diseases with major nutritional determinants Other disorders Diseases in which nutrition plays a role Digestive diseases (9.5%) Congenital abnormalities (4.2%) Nutritional endocrine disorders (2.6%) Neuropsychiatric disorders (51.1%) Perinatal conditions (8%) Respiratory diseases (13.2%) Oral diseases (1.1%) Respiratory infections (6.8%) Maternal condition (1%) Infectious and parasitic diseases (10.5%) Unintentional injury (45.9%) Intentional injury (21.9%) Genitourinary diseases (5%) Musculoskeletal diseases Skin diseases (19%) (0.1%) Sense organ disorders (0.1%) Diet and disease 9 including dietary factors, in the EU (6), and ranked the leading risk factors contributing to the burden of disease (Table 1.1). Analyses suggest that poor nutrition accounts for 4.6% of the total DALYs lost in the EU, with overweight and physical inactivity accounting for an additional 3.7% and 1.4%, respectively (6). This analysis does not, however, capture the complexity of the situation and is thus likely to underestimate the importance of nutrition. For example, dietary factors interact with other risk factors. Substantial fruit and vegetable consumption seems to reduce the risk of lung cancer among smokers, although smoking is associated with a large increase in the probability of developing lung cancer even among those with the highest consumption. Other dietary components may moderate the impact of alcohol consumption. Taken together, this evidence suggests that improving nutrition could be the single most important contributor to reducing the burden of disease in the WHO European Region. Table 1.1. Contribution of selected factors to the overall burden of disease in the EU Source: Determinants of the burden of disease in the European Union (6). Studies from Australia and New Zealand (7–9) support this finding. In these countries, about 3% of the burden of disease (2.8% in Australia and 2–4% in New Zealand) could be attributed to low consumption of fruits and vegetables. The Australian studies also reported that about 10% of all cancer cases could be attributable to insufficient intake (8,9). The contribution of various factors to the total burden of disease has been estimated in Australia (8) (Fig. 1.2). The multiple interacting processes by which different dietary factors contribute to the disease burden make these analyses more difficult, and there is no agreement on the extent of synergism or on the relative quantitative importance of the main contributors to different diseases or to public health in general. Causal factor Contribution (%) Tobacco smoking 9.0 Alcohol consumption 8.4 Overweight 3.7 Occupational risks 3.6 Low fruit and vegetable consumption 3.5 Relative poverty 3.1 Unemployment 2.9 Illicit drugs 2.4 Physical inactivity 1.4 Diet high in saturated fat 1.1 Outdoor air pollution 0.2 10 Food and health in Europe Fig. 1.2. Proportion of the total burden of disease (in DALYs lost) attributable to selected risk factors, by sex, Australia, 1996 Source: adapted from Mathers et al. (8). CVD and cancer cause almost two thirds of the overall burden of disease in Europe. Conservative estimates suggest that about one third of CVD is related to inappropriate nutrition, although the need for more research is widely acknowledged. Cancer kills about 1 million adults each year in the WHO European Region. As with CVD, inappropriate diet causes about one third of all cancer deaths worldwide. A report by the World Cancer Research Fund and the American Institute for Cancer Research (10) estimated that improved diet, along with maintenance of physical activity and appropriate body mass, could reduce cancer incidence by 30–40% over time. Doll & Peto (11) made a widely cited estimate of the diet-related burden of cancer, attributing about 35% of all cancer deaths in the United States to diet (excluding alcohol) and a further 3% to alcohol. They qualified this, however, by also suggesting a range of plausible estimates of between 10% and 70% attributable to diet and a further 2.4% to alcohol. Doll (12) later proposed that the evidence available up to the early 1990s associating diet with cancer had become stronger, and gave a narrower range of 20–60%. Numerous studies have aimed to identify the components of diet that have the greatest influence on CVD and cancer. Many earlier clinical and epidemiological investigations focused on fat intake. In the early 1990s, a study in the United States suggested that reducing fat consumption from 37% of energy intake to 30% would prevent 2% of deaths from CVD and cancer, primarily among people older than 65 years (13). More recently, High blood cholesterol High blood pressure Lack of fruit and vegetables Obesity Physical inactivity Alcohol harm Alcohol benefit Tobacco Illicit drugs Occupational Unsafe sex –4 –2 0 2 4 6 8 10 12 14 Percentage of total DALYs Males Females Total = 15% Diet and disease 11 Willett (14) suggested that replacing saturated and trans-fatty acids in the diet could be more important for preventing CVD than reducing the total amount of fat consumed. For example, replacing 6% of energy intake from predominantly animal fat with monounsaturated fat could potentially reduce CVD by 6–8% (15). Growing evidence also indicates that other dietary factors are associated with CVD and cancer risk. There is an international consensus that an excess of energy (more energy consumed in the diet than is expended) and alcohol are risk factors for certain types of cancer (mouth, pharynx, larynx, oesophagus and liver) and that a high intake of fruits and vegetables protects in part against the agents causing cancers of the mouth, pharynx, oesophagus, stomach and lung (10,16,17). Deficiencies of substances such as vitamin A, other antioxidant vitamins and non-nutrient components of fruits and vegetables have also been linked to an increased risk of both CVD and cancer, although this area remains inadequately researched (10,18). Joffe & Robertson (19) investigated the potential health gain if vegetable and fruit intake increased substantially within the EU and three countries in the process of joining it. They estimated that about 23 000 deaths from coronary heart disease (CHD) and major types of cancer before age 65 could be prevented annually if low intake of fruits and vegetables were increased to that of the groups consuming the most. The importance of nutrition in determining or modulating so many major causes of disability and premature death implies that dietary patterns should differ remarkably across Europe and change over time. Fig. 1.3 displays the remarkable variation in estimated national intake of fruits and vegetables in the EU countries, the Czech Republic, Hungary and Poland. There is a general north–south gradient, with higher intake in the south. The WHO goal for vegetable and fruit intake is at least 400 g per person per day as a national average throughout the year (21). The intake is less than this in most countries in the European Region, although climate and agricultural conditions in southern and central Europe are ideal for producing sufficient fruits and vegetables to feed the whole Region throughout the year. The mean consumption of fruits and vegetables is a poor measure of the distribution of intake within a population. Fruit and vegetable intake is not normally distributed evenly, but highly skewed. Thus, the mean intake values conceal a large proportion of the population within each country with very low consumption. Despite a relatively high mean consumption of 500 g per day in Greece, for example, 37% of the population is below the recommended level (22). The availability of fruits and vegetables differs vastly at different times of year. Powles et al. (23) found evidence for the importance of seasonality in the role of fresh fruits and vegetables in reducing CVD mortality. This has been 12 Food and health in Europe suggested as one explanation for the seasonal cycling and severity of CHD in the affected countries (23). Fig. 1.3. Vegetable and fruit intake (mean g/day) in selected European countries Source: Comparative analysis of food and nutrition policies in the WHO European Region 1994–1999. Full report (20). Not only does fruit and vegetable intake differ surprisingly across Europe, but both the total quantity eaten and the variety and choice have changed remarkably over the last 50 years. Similar changes and differences apply to the availability of milk fat and fish (according to food balance sheets of the Food and Agriculture Organization of the United Nations (FAO) – Fig. 1.4 and 1.5). Consumption of milk fat is very substantial in north-western Europe and especially in the non-Mediterranean countries. Given its major contribution in inducing high serum cholesterol levels and CVD, it is not surprising that milk-fat consumption predicts the prevalence of CVD across Europe (24). 0 100 200 300 400 500 600 700 United Kingdom (1995) Ireland (1989) Austria (1998) Netherlands (1992) Germany (1990) Czech Republic (1997) Sweden (1989) Denmark (1995) Poland (1997) Belgium–Luxembourg (1982) Hungary (1997) Portugal (1980) France (1996) Italy (1995) Finland (1997) Greece (1997) Spain (1994) Intake (g per person per day) WHO goal Diet and disease 13 Fig. 1.4. Availability of milk fat, selected countries in the WHO European Region, 1998 a The former Yugoslav Republic of Macedonia. Source: Food and Agriculture Organization of the United Nations (http://apps. fao.org/lim500/wrap.pl?FoodBalanceSheet&Domain=FoodBalanceSheet&Language=english, accessed 25 September 2003). The pattern of fish supply shown in Fig. 1.5 may result from the availability of fish in the locality unless a country is affluent enough to import substantial quantities. If an intake of at least 200 g fish per person per week is considered reasonable, consumption reaches this level in only about 10% of countries. 6 10 10 12 8 12 12 12 3 13 11 15 16 16 12 13 18 16 14 15 15 16 20 12 21 18 17 21 23 16 26 16 17 28 16 22 26 24 21 26 23 24 24 3 1 2 1 5 1 1 2 11 3 5 1 1 1 6 5 1 2 5 4 4 4 9 1 5 10 7 6 13 3 13 12 1 15 9 5 8 11 10 14 13 20 0 5 10 15 20 25 30 35 40 45 50 Armenia Azerbaijan Lithuania Uzbekistan TFYR Macedonia Turkmenistan Spain Slovakia Bulgaria Ukraine Latvia Malta Romania Poland Norway Greece Belarus Germany Netherlands Austria Switzerland France Iceland Finland Ireland Sweden Albania Belgium–Luxembourg Estonia United Kingdom Italy Czech Republic Denmark Portugal Slovenia Russian Federation Kyrgyzstan Kazakhstan Hungary Israel Croatia Republic of Moldova Georgia Milk fat Butter Availability (g per person per day) a 14 Food and health in Europe Fig. 1.5. Availability of fish, selected countries in the WHO European Region, 1998 Source: Food and Agriculture Organization of the United Nations (http://apps. fao.org/lim500/wrap.pl?FoodBalanceSheet&Domain=FoodBalanceSheet&Language=english, accessed 25 September 2003). Government policies and industry initiatives can substantially affect the national consumption of all three categories of food considered here. For instance, when eastern Finland and the province of North Karelia were especially affected by CVD, a major comprehensive prevention project was started in 1972, and developed from a demonstration project into national action. Legislative and other policy decisions included the development of low-fat spreads, fat and salt labelling for many food groups and improving the quality of meals at schools and in the army. The food industry became involved by developing a cholesterol-lowering rapeseed oil from a new type of rape plant that grows well in the northern climate of Finland. This was in effect a domestic, heart-healthy alternative to butter. As a result, from 1972 to 1997, vegetable 0 50 100 150 200 250 300 Uzbekistan Republic of Moldova Belarus Romania Turkmenistan Kazakhstan Croatia TFYR Macedonia Slovenia Czech Republic Austria Germany Netherlands Switzerland Belgium–Luxembourg United Kingdom Israel Greece France Malta Norway Iceland Portugal Spain Finland Sweden Denmark Italy Russian Federation Estonia Lithuania Ireland Poland Latvia Ukraine Slovakia Hungary Bulgaria Georgia Albania Azerbaijan Armenia Kyrgyzstan Availability (g per person per day) a The former Yugoslav Republic of Macedonia. a Diet and disease 15 intake nearly tripled; fish consumption doubled; the use of full-fat milk fell dramatically (Fig. 1.6) and vegetable oil increasingly replaced butter (Fig. 1.7). Fig. 1.6. Percentage of men and women aged 35–59 years in North Karelia, Finland drinking fat-containing milk and skim milk, 1972 and 1997 Source: Puska (25). Fig. 1.7. Percentage of men and women aged 35–59 years in North Karelia, Finland using butter and vegetable oil, 1972 and 1997 Source: Puska (25). These comprehensive actions were associated with a remarkable fall in CVD mortality, especially CHD mortality, in eastern Finland (Fig. 1.8). These differences in intake of fruits and vegetables, fish and milk fat can be linked to other nutritional problems. Thus, pregnant women eating more fruits and vegetables have a higher intake of folic acid; this has been linked to fewer small and premature babies and to the prevention of neural tube defects (see p. 47). Women’s consumption of fruits and vegetables limits the likelihood of iron deficiency before pregnancy and of developing anaemia in pregnancy. 0 10 20 30 40 50 60 70 80 90 Men Women Men Women 1972 Use of fatty milk (%) 0 5 10 15 20 25 Men Women Men Women 1972 Use of skim milk (%) 1997 1997 0 10 20 30 40 50 60 70 80 90 Men Women Men Women 1972 1997 Use of butter on bread (%) 0 5 10 15 20 25 30 35 40 Men Women Men Women 1972 1997 Use of vegetable oil for cooking (%) 16 Food and health in Europe In addition, the fruits and vegetables eaten by a nursing mother induce higher blood levels of water-soluble vitamins, which readily pass to the breastfed baby. Fig. 1.8. Predicted and observed mortality from CHD in females aged 35–64, north-eastern Finland Source: Vartiainen et al. (26). The consumption of vegetables and fish by young women before and during pregnancy is also crucial to storing omega-3 essential fatty acids in their fat depots, which are called on selectively during pregnancy for channelling to the uterus and the developing fetus. The growth of the fetus and especially the brain of both the fetus and young child crucially depend on having adequate amounts of omega-3 essential fatty acids, which happens only if the mother has been eating an appropriate diet and breastfeeding her child. WHO advocates the gradual introduction of a variety of puréed fruits and vegetables and fish and meats at about 6 months (see Chapter 4, pp. 245–248) (27). Unmodified cow’s milk should not be given as a drink before the age of 9 months but can be used in small quantities in preparing complementary foods for babies aged 6–9 months (see Chapter 4, pp. 245–248). Fish not only is a good source of omega-3 fatty acids but also modulates immune responsiveness, limits disturbances of fat metabolism and stabilizes Decline in mortality (%) Year 1972 1976 1980 1984 1988 1992 Smoking Blood pressure Predicted (all risk factors) Cholesterol Observed (all risk factors) –20 0 20 40 60 80 Diet and disease 17 the excitability of the heart, thereby limiting the risk of sudden cardiac death. Moreover, fish provides an excellent source of zinc, iron and animal proteins that are conducive to the longitudinal growth of the child and the prevention of anaemia. Given this remarkable interplay between different foods and health, why is the European population not consuming enough of these vital foods at every stage of the life-course? What are the main impediments to their availability and consumption? The precise reasons for poor intake need to be assessed in each country and for each age group, but this book discusses general possibilities in the section on social inequality in this chapter (see pp. 66–73) and gives policy options in Chapter 4. The widely varying dietary patterns across Europe are governed by not only geographical, climatic and agricultural factors described in Chapter 3 (see Fig. 3.5, p. 166) but also societal conditions, including income levels, civil strife, the status of women, urbanization, exposure to marketing and the changing of family and community structures. The nutrition transition and its effects on health National consumption figures for fruits and vegetables and other dietary ingredients (Fig. 1.3–1.5) and breastfeeding rates (see Fig. 1.23, p. 51) differ remarkably. Consumption levels can change over relatively short periods, as shown by the decline in milk-fat consumption in parts of Finland. Comparison of dietary patterns with other national statistics, such as gross national product, suggests that consumption patterns for dietary components such as meat, fat and vegetables are linked to national wealth, but these patterns change over time and, at the level of households, may depend on income and food security. At a global level, good evidence indicates a transition in nutrition, in which rising national wealth is accompanied by changes in diet, with an increase in consumption of animal-derived products, fat and oil and a reduction in cereal foods and vegetables. The WHO publication Globalization, diets and noncommunicable diseases (28) describes this transition: Rapid changes in diets and lifestyles resulting from industrialization, urbanization, economic development and market globalization are having a significant impact on the nutritional status of populations. The processes of modernization and economic transition have led to industrialization in many countries and the development of economies that are dependent on trade in the global market. While results include improved standards of living and greater access to services, there have also been significant negative consequences in terms of inappropriate dietary patterns and decreased physical activities, and a corresponding increase in nutritional and diet-related diseases. 18 Food and health in Europe Food and food products have become commodities produced and traded in a market that has expanded from an essentially local base to an increasingly global one. Changes in the world food economy have contributed to shifting dietary patterns, for example increased consumption of an energy-dense diet high in fat, particularly saturated fat, and low in carbohydrates. This combines with a decline in energy expenditure that is associated with a sedentary lifestyle, with motorized transport, and labour-saving devices at home and at work largely replacing physically demanding manual tasks, and leisure time often being dominated by physically undemanding pastimes. Because of these changes in dietary and lifestyle patterns, diet-related diseases – including obesity, type II diabetes mellitus, cardiovascular disease, hypertension and stroke, and various forms of cancer – are increasingly significant causes of disability and premature death in both developing and newly developed countries. They are taking over from more traditional public health concerns like undernutrition and infectious disease, and placing additional burdens on already overtaxed national health budgets. Dietary patterns, based on food supply data, can be estimated for national populations, using the FAO database, from 1960 onwards. A pattern of nutrition transition can be detected in, for example, southern European countries, which traditionally had diets dominated by plant foods, fish, olive oil and wine. Countries such as Greece, Portugal and Spain show some evidence of moving from Mediterranean-type diets to ones more like those eaten in northern Europe, rich in meat and dairy products. Simopoulos & Visioli (29) suggest that there is not one type of Mediterranean diet, although countries of the Mediterranean region traditionally all have high intakes of fruits and vegetables and low intakes of saturated animal fat. The region includes varied cultures, traditions, incomes and dietary habits and patterns, all of which are evolving with the impact of economic development and globalization. The food supplies and therefore the diets of Europeans seem to be changing rapidly. The demographic transition – from rural societies with low life expectancy at birth and families with many children to urban societies with higher life expectancy at birth and fewer children – is well known. The epidemiological transition that follows the demographic transition is also fairly well understood: a shift from endemic deficiency and infectious diseases, mostly in early life, to chronic diseases in later life. Evidence is now sufficient to propose a general theory for these causally and chronologically linked demographic, nutrition and epidemiological transitions. When populations undergo massive social and technological change – as in the NIS, where the level of urbanization is predicted to reach 90% by 2015 – their food supplies and thus disease patterns also change. This pattern Diet and disease 19 can be traced in more economically developed countries, such as the United Kingdom, between the sixteenth and eighteenth centuries following the agrarian and industrial revolutions. In the CCEE and NIS, such transitions are taking place very much faster and in some cases extremely rapidly. This has immense implications for policy-making in public health. The nutrition transition is marked by a shift away from diets based on indigenous staple foods, such as grains, starchy roots and locally grown legumes, fruits and vegetables, towards more varied diets that include more processed food, more foods of animal origin, more added sugar, salt and fat, and often more alcohol. This shift is accompanied by reduced physical activity in work and leisure. Combined, these changes leading to a rapid increase in obesity and its associated health problems. Consequently, in most countries of the European Region, diet-related diseases are gaining in magnitude and effects compared with the effects of specific dietary deficiencies, even though certain micronutrient deficiencies (in, for example, iodine and iron) are still prevalent. If appropriate public policies are not implemented to change the transition patterns, these public health problems are likely to continue into future generations. Costs to the health care system Information is needed on the cost of diseases attributable to diet and the burden they place on society. It can be valuable in risk management (evaluating the benefits and costs of adopting certain risk control measures or health interventions) and in assessing the impact of ill health on national economies and health service budgets. In the early 1990s, the Federal Ministry of Health estimated the total costs of diet-related diseases to the health service in Germany at about DM 83.5 billion (Table 1.2), equivalent to 30% of the total cost of health care. The costs include both direct costs (medical and health service expenditure) and indirect costs (from workers’ reduced productivity or lost family income). The highest costs resulted from CVD (12% of the total national health care costs), followed by dental caries (7%) and diet-dependent cancer (3%) (30). In the United Kingdom, Liu et al. (31) estimated that CHD cost £1.65 billion to the health care system, £2.42 billion in informal care and £4.02 billion in productivity loss: a total annual cost of £8.08 billion. This made CHD the most expensive disease in the United Kingdom for which comparable analyses have been done, including back pain, rheumatoid arthritis and Alzheimer’s disease. Liu et al. (31) also noted considerable variation in both the direct health care costs and the productivity and informal care costs per 100 000 CHD patients in different countries. Unsurprisingly, given the different levels of provision and of unit costs, they observed that the direct health and social care 20 Food and health in Europe costs of CHD were considerably lower in the United Kingdom than in other countries for which data were available. The direct costs were about 1.2 times higher in the Netherlands, 5.5 times higher in Sweden and 6 times higher in Germany. In contrast, the employment and informal care costs in the United Kingdom were higher than those in Switzerland and were very similar to those in Sweden or Germany. Table 1.2. Costs of diet-dependent conditions in Germany, 1990s Source: adapted from Kohlmeier et al. (30). Kenkel & Manning (32) summarized studies by the National Institutes of Health and by Wolf & Colditz (33) of the costs of illnesses associated with dietary factors and physical activity patterns in the United States. The illnesses included CHD, diabetes, stroke, osteoporosis, gall bladder disease and cancers of the breast, colon/rectum and prostate. The estimates are based on the assumption that dietary factors and sedentary lifestyles contribute to 60% of diabetes cases; 35% of breast, colon/rectum and prostate cancer cases; 30% of gall bladder disease; 25% of arthritis; and 20% of CHD and stroke. The total economic cost of all these diet- and exercise-related illnesses was estimated at US $137 billion (32): more than the economic costs of alcohol abuse and dependence (US $118 billion) or smoking (US $90 billion). The direct costs of diet- and exercise-related illnesses – health care expenditure attributable to these conditions – reached US $67 billion, or about 7% of total personal health care expenditure in the United States. Also in the United States, Oster et al. (34) suggested that a sustained 10% weight loss among obese people would lead to a lifetime saving of US $2200– Conditions Estimated costs (DM billion) Total Direct Indirect CVD 32.9 15.4 17.6 Dental caries 20.2 20.2
- This may complicate the picture, because some processing methods may contribute to the increased risk. Fig. 1.14. Dose–response relationship between the consumption of red and processed meat and the risk of colorectal cancer Source: Norat et al. (72). Reprinted by permission of Wiley-Liss, Inc, a subsidiary of John Wiley & Sons, Inc. Some evidence indicates that diets containing substantial amounts of meat may increase the risk of cancer of the pancreas, breast, prostate and kidney. This evidence is weaker than that linking meat to colorectal cancer and was classified by the World Cancer Research Fund as “possible” (10). Average meat intakes do not vary as much across the European Region as vegetable intakes. Nevertheless, countries show considerable variation in the types of meat consumed and the method of processing used, so national policy-makers should assess their own country’s trends. Overweight and increased risk A WHO review of the literature linking body weight to the risk of cancer at various sites (35) suggests that convincing evidence links excess weight to an elevated risk of endometrial cancer. Good evidence links excess weight to kidney cancer and breast cancer in post-menopausal women (10). The review (35) also noted possible links between raised body weight and an elevated risk of colorectal cancer and between high energy intake and pancreatic cancer. A recent meta-analysis connected overweight with increased risk of cancer of the kidney, endometrium, colon/rectum, prostate, gall bladder and (in post-menopausal women) breast (73). This study also estimated the 0.5 0 20 Consumption (g/day) Red meat (all) Meat (all) Red meat (fresh) Meat (fresh) Processed meat Relative risk 40 60 80 1 1.5 2 Diet and disease 35 proportion of cancer in the EU attributable to excess weight. Overall, it accounts for 5% of all cancer cases in the EU: 3% in men and 6% in women, corresponding to cases in over 25 000 males and 44 000 females each year. This included over 21 600 cases of colorectal cancer, 14 200 cases of endometrial cancer and 12 800 cases of breast cancer. On this basis, halving the numbers of people in the EU who are overweight and obese might prevent some 36 000 cases of cancer each year (73). Epidemic of overweight and obesity The problem of overweight and obesity has only recently come to the forefront of public health, as public health nutritionists were primarily concerned with the problems of undernutrition, especially in vulnerable groups in society. WHO, however, calls overweight (a body mass index – BMI2 – of 25–29.9) and obesity (BMI of 30 or more) the biggest unrecognized public health problem in the world; they contribute substantially to both ill health and death in populations (1). Excess weight is calculated to be responsible for nearly 300 000 deaths annually in the EU – nearly 1 in 12 of all deaths recorded – by contributing to CVD and cancer (74). The major complications of excess weight are type 2 diabetes, high blood pressure, CHD, stroke, a range of cancer types and arthritis. A series of disabilities and psychological problems are linked directly to excess weight. Evidence is accumulating that the emerging epidemic of overweight and obesity in children is markedly amplifying the early onset of other health problems, especially type 2 diabetes. In addition, the risk of gestational diabetes increases in obese pregnant women; this increases the risk of subsequent fetal defects, childhood obesity and diabetes (see pp. 37–38). Recent data sets suggest that many European countries have some of the highest national rates of overweight and obesity among children (75) and adults in the world. The prevalence of obesity is increasing in all age groups in most European countries. Obesity is a rapidly growing epidemic, now affecting about 30% of the population of the WHO European Region (76). Published and unpublished data from studies and surveys by WHO and others (73,76–91) show that a considerable proportion of the adult population in many European countries is overweight or obese; Fig. 1.15 and 1.16 arrange these data for groups of countries in the Region. Overweight levels range from 9% to 41% of women and 10% to 50% of men. Further, the trend of overweight is consistently rising, although the rate of increase 2 BMI is one’s weight in kg divided by (height in metres)2 . 36 Food and health in Europe varies. Even the Scandinavian countries, with historically more active populations relative to many other countries, have been affected. Fig. 1.15. Overweight adults (BMI 25–29.9), European Region (%) a No data are available on overweight in men. Special risks of abdominal obesity The distribution of excess fat in the body has been recognized as an important predictor of ill health. Excess intra-abdominal fat is linked to a range of health hazards, including diabetes, a greater propensity to hypertension and dyslipidaemia and an increased risk of CHD and stroke. This array of problems is specified as the metabolic syndrome or syndrome X, which is also associated with excessive kidney albumin excretion. This condition is especially seen in men, is amplified by drinking and smoking and has also been linked to mental stress and a programming of fat distribution and disease by poor early fetal and childhood development (92). In women, abdominal obesity is associated with polycystic ovarian syndrome, infertility, menstrual abnormality and hirsutism. Abdominal obesity can be simply assessed by measuring the waist circumference, and WHO has proposed limits (see Chapter 4, p. 240) for the waist circumference of men and women based on the risk of blood pressure, diabetes and blood lipid abnormalities derived from a population study in the Netherlands (93). There is a new emphasis on highlighting the significance of Uzbekistan Kyrgyzstan Russian Federation Latvia Lithuania Turkey Greece Malta Spain Portugal Israel France Switzerland Netherlands Germany United Kingdom Austria Belgium Sweden Denmark Norway Finland Yugoslavia Bulgaria Hungary Romania Slovakia Czech Republic Kazakhstan 60 40 20 0 20 40 60 Percentage a Men Women Italy a a Diet and disease 37 waist measurements because this can be used in campaigns to alert adults to the problems of weight gain and the particular risk of abdominal obesity. It could also give an early warning to physicians of the likelihood of disease developing in their patients. Implications of childhood obesity It is now recognized that large infants (those weighing more than 4 kg at birth) are more likely to develop obesity in later childhood and that low-birthweight infants who grow very rapidly after the age of 1 year and become overweight are more likely to develop CVD in adult life. Subsequent studies have not borne out the original concern about fat infants being doomed to become overweight and obese adults. The risk of a child persisting with overweight and obesity, however, increases progressively from the age of about 6 years. The prevalence of overweight and obesity among children in Europe is rising significantly, with up to 27% affected in some regions (75). In examining overweight in preschool children from over 90 countries, de Onis & Blossner (94) used the standard WHO procedure of defining overweight as a BMI exceeding 2 standard deviations (SD) above the median for the WHO international growth charts. They found overweight children in all the 11 countries in the European Region examined: Armenia, Fig. 1.16. Obese adults (BMI >30), European Region (%) a No data are available on obesity in men. 40 30 20 10 0 10 20 30 40 Czech Republic Slovakia Romania Hungary Bulgaria Yugoslavia Finland Norway Denmark Sweden Belgium United Kingdom (England) Germany Netherlands Switzerland France Israel Portugal Spain Italy Malta Greece Turkey Lithuania Latvia Russian Federation Kazakhstan Kyrgyzstan Uzbekistan Men Women Percentage a a a 38 Food and health in Europe Azerbaijan, Croatia, the Czech Republic, Hungary, Italy, Kazakhstan, Turkey, the United Kingdom, Uzbekistan and Yugoslavia. The prevalence in eastern countries was, for example, 6% overweight young children in Armenia and about 15% in Uzbekistan (94). In addition, about 20% of preschool children in the Russian Federation were overweight in 1997 (http://www.who.int/ nutgrowthdb/intro_text.htm, accessed 19 September 2003). The major problem associated with childhood and adolescent obesity is its persistence into adult life and its association with diabetes and CVD risk in later life (95). Thus, the problem of obesity in children is arousing intense concern and increasing political attention. Type 2 diabetes and excessive weight gain Type 2 diabetes occurs when insulin secretion is insufficient to overcome resistance to its action, leading to inadequate regulation of blood glucose levels. This is the underlying abnormality in most cases with this condition. It was previously a disease of middle-aged and elderly people, but its frequency has escalated in all age groups and the condition is now seen in adolescence and childhood. The prevalence of type 2 diabetes is expected to increase to more than 10% in all EU and Nordic countries. In addition, the rate of increase is projected to rise dramatically by 2025 (76). Diabetes rates have risen in parallel with those of overweight and obesity. Powerful evidence indicates that excess weight, especially when centrally distributed, and physical inactivity increase insulin resistance and are independent determinants of diabetes risk. This risk increases even with modest weight increases within the normal range (BMI under 25). A high intake of saturated fatty acids increases insulin resistance and the risk of type 2 diabetes. Weight loss in overweight and obese people, increased physical activity and reduced saturated fat intake have been convincingly shown to reduce the risk of insulin resistance and diabetes. Impact of physical inactivity on health Evidence is increasing that regular physical activity has considerable health benefits, such as reducing the risk of CVD, diabetes and osteoporosis (96). In comparison with sedentary people, physically active people (96): • run 50% less risk of dying from CHD and stroke; • are at lower risk of hip fracture (30–50%), hypertension (30%), colorectal cancer (40–50%) and type 2 diabetes (20–60%); • are 50% less likely to become obese; Diet and disease 39 • have a 25–50% lower risk of developing functional limitations in later life; and • show a 50% slower decrease of aerobic capacity (which occurs with age), thereby gaining 10–20 years of independent living. Physical activity plays a role in avoiding overweight and obesity: people with low levels of physical activity have higher body fat and abdominal fat and are more likely to gain body fat than those with high levels of physical activity (97). Physical activity also contributes to maintaining a lower blood pressure throughout life and to lowering the ratio of LDL to HDL cholesterol in the blood. The benefits of physical activity explain its substantial importance in limiting death and illness from CVD. Assessing physical activity levels, Currie et al. (98) found that children exercise progressively less as they grow older. The proportion of 15-year-olds who reported taking part in sports outside school at least twice a week ranged from 37% to 66% in girls and from 60% and 90% in boys (Fig. 1.17). Fig. 1.17. Proportion of 15-year-olds who report exercising vigorously twice a week or more, European Region Source: Currie et al. (98). 100 80 60 40 20 0 20 40 60 80 United Kingdom (Northern Ireland) Austria United Kingdom (Scotland) Germany United Kingdom (Wales) Switzerland Ireland United Kingdom (England) Belgium (Flanders) France Estonia Lithuania Latvia Czech Republic Poland Hungary Greece Portugal Israel Russian Federation Finland Norway Sweden Denmark Denmark (Greenland) Percentage Boys Girls 40 Food and health in Europe Associations between physical activity and socioeconomic status have been observed in schoolchildren, with children from lower-status families taking less exercise on average than those from higher-status families, and, in Germany and the United Kingdom at least, undertaking less physical activity outside school (99,100). The survey in Germany involved 3400 children aged 5–7 years and showed that lower physical activity was associated with lower educational status of the family and with unhealthy eating patterns (100). It also found that children watching more than 1 hour of television per day ate significantly more confectionery and fast food than children watching less (100). A later section in this chapter deals with physical activity and inequalities (see pp. 71–72). The data on physical activity among European adults are poor. A survey of adults in the EU shows that levels of activity are low; on average 32% of adults carry out no leisure-time physical activity in a typical week (101). In general, southern EU countries have lower levels of physical activity than northern and western countries (101). Physical activity contributes to physical, mental and social health and improves the quality of life of people of all ages. These benefits also help to reduce social and health care costs (102). Physical activity should be considered an essential element of preventing chronic disease, as well as a central part of a healthy lifestyle. Policy-makers’ recommendations must address physical activity in children, adolescents, adults and older people and particularly must involve employers and schools, as this is instrumental to making successful policies (see Chapter 4, pp. 238–239). Impaired infant and child development from micronutrient deficiency Iodine deficiency Iodine deficiency leads to what are collectively called iodine deficiency disorders, and is the primary cause of avoidable mental deficiency in childhood. The most severe forms of these disorders can result in cretinism or severe brain damage. In children and adolescents, iodine deficiency leads to overt or subclinical hypothyroidism, impaired mental and physical development, and goitre. A comprehensive WHO report on iodine deficiency disorders and their control (103) presents an overview of the situation in the European Region. Mild and moderate forms of iodine deficiency are still common in Europe (104), with neurological defects and minor impairments of brain functioning evident. According to the WHO global database on iodine deficiency disorders, they are estimated to affect about 130 million people in the Region. Iodine deficiency disorders are considered unlikely in a number of European countries: Austria, Finland, Ireland, Monaco, the Netherlands, Diet and disease 41 Norway, San Marino, Sweden, Switzerland and the United Kingdom (105). Nevertheless, recent surveys of the prevalence of goitre show that many people in the European Region still suffer from moderate iodine deficiency. (The prevalence of goitre only reveals a proportion of the iodine deficiency problem, however, and insufficiency of iodine is likely to be much higher.) For example, the prevalence of goitre was 11% for adults in Azerbaijan in 1996 and 37% for the population of Uzbekistan in 1998. Fig. 1.18 shows the prevalence in school-age children (105). In addition, iodine deficiency disorders are still a public health problem in some western European countries, such as Belgium (105) and Italy (106). Fig. 1.18. Prevalence of goitre in school-age children in selected countries in the European Region Note: The data for the Republic of Moldova, Slovakia, Slovenia and Turkey are taken from the country responses to a 1998 WHO questionnaire on iodine deficiency disorders, not official survey reports, so they should be treated as preliminary. Source: WHO global database on iodine deficiency disorders, Geneva, World Health Organization and de Benoist & Allen (105). Iodine deficiency is easy to eradicate, but this has not yet happened in Europe. Policy-makers should implement the universal iodization of salt in their countries (see Chapter 4, p. 250). Iron deficiency Iron deficiency can result in impaired brain development in children and poor mental concentration and cognitive performance in both children and adults. In addition, iron deficiency anaemia compromises adults’ work capacity. Republic of Moldova (1996) Turkey (1980–1988) Poland (1992–1993) Bulgaria (1998) Croatia (1997) Slovenia (1996) Hungary (1999) Belgium (1998) Slovakia (1994) Prevalence (%) 0 5 10 15 20 25 30 35 40 42 Food and health in Europe The body needs iron as a component of a variety of enzyme systems in all tissues and for the production of blood haemoglobin, crucial for the transport of oxygen. Dietary iron in its normal inorganic form is poorly absorbed by the intestine because of the interaction of a variety of dietary inhibitors, which bind the iron and reduce its bioavailability to 3–15% (see Chapter 4, pp. 251–252). Bioavailability is much improved when iron is consumed with vitamin C from fruits and vegetables or when dietary iron is eaten in the organic form, for example, as part of the haem iron protein found in meat and fish. Important compounds in vegetable foods interfere with iron bioavailability: the phytates found, for example, in unrefined grains; the albumin from eggs; and the polyphenols and other compounds found in tea. Fruits and vegetables rich in vitamin C limit the impact of phytates. Calcium and zinc intake may also modify iron bioavailability. A variety of factors can cause iron deficiency and anaemia: insufficient dietary iron, dietary anti-nutrients (such as phytates and polyphenols), blood loss and intestinal parasites, especially helminths such as hookworm, and gastrointestinal infections. Pica – the craving for non-food items such as soil and chalk – is still claimed to be quite prevalent in certain parts of Europe. Pica can occur during pregnancy, and the unusual items eaten amplify the malabsorption of iron (107), leading to iron deficiency anaemia. In the European Region, infants and children may develop iron deficiency anaemia from poor feeding practices, such as giving tea to infants and children, or when weaning off breast-milk does not coincide with the introduction of fruits and vegetables, along with meat and fish. Prematurity exacerbates the problem of anaemia because iron stores are limited in a small newborn baby; any infestation with parasites or helminths, as a result of poor hygiene and impure water, markedly exacerbates the problem by amplifying malabsorption and stimulating excessive intestinal blood loss. In addition to poor feeding practices, low breastfeeding rates can be considered a major cause of iron deficiency anaemia in infants and young children. Very high prevalence has been reported from the central Asian republics (80,82,108,109), Bosnia and Herzegovina (110) and parts of western Europe (111). Even in affluent countries, such as the United Kingdom, the prevalence in children of Asian background has been observed to be 12% in those aged 1–2 years and 6% in those aged 2–4 years (111). Children in other countries in western Europe also show high levels of iron store depletion (112). In addition, many adolescents in Europe have either iron deficiency anaemia or depleted iron stores (112). The latter is a precursor to the development of anaemia. Adolescent girls tend to have higher rates of iron deficiency and anaemia than boys; these are due not only to the onset of puberty, with its increased iron requirements, but also the iron loss with menstruation (113,114). Diet and disease 43 The high rates of anaemia and iron depletion among women of reproductive age in the European Region are of great concern. They can have a number of causes. Although women throughout the Region are affected, Fig. 1.19 shows that the prevalence of anaemia is highest in central Asian countries (80,82,108, 109,111,114). Evidence from Kazakhstan (115) shows that women had a relatively low mean iron intake (13.2 mg/day) and about 35% of Kazakh women of reproductive age were suffering from anaemia (haemoglobin under 12 g/dl blood) in 1999. In Sweden, over 30% of women of reproductive age have low iron stores. Fig. 1.19. Prevalence of anaemia and depleted iron storesa in women of reproductive age, selected European countries a Investigators used their own definitions of depleted iron stores (112). b The former Yugoslav Republic of Macedonia. Sources: Kazakhstan demographic and health survey (DHS), 1999 (80), Kyrgyzstan demographic and health survey (DHS), 1997 (82), Uzbekistan demographic and health survey, 1996 (109), Branca et al. (personal communication, 1996), Hercberg et al. (112) and Branca et al. (116). Significant socioeconomic deprivation can in part explain some of these high rates, although probably not those in Sweden. For example, a cohort study of 15 000 people in the United Kingdom found that women in the lowest social class were 1.5 times more likely to be anaemic that those in the highest social class (117). In pregnancy, substantial iron stores are mobilized because of the need not only to supply extra maternal tissues (such as the placenta) and the growing fetus but also to expand the woman’s blood volume. In some countries of the 65 55 45 35 25 15 5 5 15 25 35 45 55 65 Denmark France Norway Russian Federation Sweden United Kingdom (Surrey) Poland TFYR Macedonia United Kingdom (Northern Ireland) Armenia Azerbaijan Kazakhstan Kyrgyzstan Uzbekistan Anaemia Depleted iron stores Prevalence (%) b 0 44 Food and health in Europe Region, pregnant women have a high prevalence of anaemia, especially those with successive pregnancies. In such cases, the women’s bodies cannot meet the repeated high demands for haemoglobin production from their already depleted iron stores; the depletion is exacerbated by the normal iron demands of the growing fetus and the loss of blood in childbirth. The severity and prevalence of anaemia during pregnancy depend on the prevalence of pre-existing iron deficiency and anaemia. In Armenia, 50% of the women in the third trimester of pregnancy have mild or moderate anaemia (116). In Uzbekistan, 27% of pregnant women have moderate anaemia; children born to these women are also likely to be anaemic (109). Multiple pregnancies and repeated abortions worsen anaemia in women of reproductive age. In some countries, abortion is an important cause of iron depletion through blood loss, especially where rates are high and abortion is still practised as a method of birth control (118). In certain central Asian republics, the prevalence of moderate-to-severe anaemia among women with two or more births can be twice as high as that among women with fewer than two births or no pregnancies (80). Wide use of the intrauterine device (IUD) provides a further explanation for high rates of anaemia. Contraceptive pills reduce menstrual losses by half (119), while an IUD doubles menstrual iron losses (120). Data on the contraceptive methods used in central Asian republics show that the IUD is used far more often than the contraceptive pill: almost 10, 5 and 4 times more often in Uzbekistan, Kyrgyzstan and Kazakhstan, respectively (80,82,108,109). Helminth infestation, especially by hookworms, is also a major cause of anaemia. Hookworms cause chronic intestinal blood loss, leading in turn to severe anaemia. The degree of anaemia they produce is linked to their number. There is some evidence (121,122) that the burden of intestinal parasitism is high in the central Asian republics, in keeping with the lack of satisfactory sanitation and clean water supplies. A dramatic increase in Table 1.3. Incidence of worm infestation in school-age adolescents in Armenia, 1993–1997 Source: adapted from Health and health care (123). Worm type Cases per 100 000 population 1993 1994 1995 1996 1997 Pinworm 297.6 373.0 361.7 1140.1 613.6 Roundworm 106.5 120.0 110.6 519.3 284.2 Trichuris spp. 12.0 9.3 7.0 22.1 17.4 Echinococcus spp. 1.7 0.8 1.5 3.15 1.6 Diet and disease 45 intestinal worm infestation among school-age adolescents in Armenia probably resulted from the difficult socioeconomic conditions (123) (Table 1.3). Evidence suggests that women benefit more from parasite elimination than from iron supplementation, since the parasites induce intestinal blood losses and double iron requirements (124). Information is urgently needed on the severity and prevalence of parasitic conditions in the European Region, especially in the central Asian republics. A consultation organized by WHO and the United Nations Children’s Fund (UNICEF) reviewed iron deficiency in the central Asian republics (125). Contributory factors appear to include high intakes of wheat, with its well recognized iron-inhibitory phytate content. Further, substantial tea drinking and relatively low meat intake by women – for example, a mean meat intake of 50 g per day in Kazakhstan (115) – are likely to amplify the iron absorption problem. The relative importance of all these issues, however, needs to be assessed. It seems clear that dietary practices can harm women and their children and that intestinal parasitism and abortions and the use of IUDs exacerbate these problems. Pregnancy and fetal development A poor diet not only deprives the developing fetus of nutrients but can also increase the loss of nutrients from the mother’s body. Several risk factors can harm a woman’s health during pregnancy. For example, teenage pregnancy puts a double nutritional burden on the body. While the adolescent has to meet increasing needs for nutrients for her own growth and development, the extra needs of the fetus jeopardize the nutritional health of both. Teenage pregnancy is a serious issue, especially in the CCEE and NIS; Fig. 1.20 shows that rates vary more than fivefold between countries in the Region (126,127). Adolescent pregnancy exposes both mother and child to adverse health and socioeconomic consequences, especially if the mother is not tall and has only modest reserves of nutrients. These conditions are especially likely to occur in the central Asian republics and Turkey (114). Pregnancy among teenagers warrants special attention, as young mothers and their children are at a higher risk of food insecurity and social and health problems. Children born to young mothers in the Region tend to have higher levels of illness, and their children, higher rates of death (80). Another important aspect of pregnancy is the need for a sufficient intake of micronutrients, especially iron, folates and iodine. Micronutrient malnutrition may begin in utero and depends largely on the mother’s nutritional status. Deficiencies retard intrauterine development and growth, which may persist through the first 2 years and permanently impair the child’s cognitive 46 Food and health in Europe development and other functions later in life. Even if micronutrient deficiencies are corrected in later childhood, the early consequences cannot be corrected, and may perpetuate the problem of stunted growth from one generation to the next. Fig. 1.20. Adolescent pregnancy rates per 1000 women aged 15–19 years in groups of European countries, 1990s Note: Data on live births and abortions are taken together to represent pregnancy rates. The unweighted average teenage birth rate in the EU dropped from 16.1 to 12.3 per 1000 women aged 15–19 years between 1990 and 1995. Birth and abortion data for the EU refer to 1990, however, since no more recent abortion data are available for some countries. No abortion data are published for several EU countries, usually because abortion is legal only in particular circumstances. For Albania, data on births refer to 1997, and data on abortions to 1995. Data for Tajikistan come from 1995; for Yugoslavia, data on abortions refer to 1996. Source: Young people in changing societies (126) and Micklewright & Stewart (127). 0 5 10 15 20 25 30 35 40 45 50 55 60 65 70 75 80 Estonia Latvia Lithuania Tajikistan Kyrgyzstan Kazakhstan Uzbekistan Russian Federation Belarus Georgia Azerbaijan Armenia Bulgaria Romania Hungary Slovakia Czech Republic Yugoslavia Albania Slovenia United Kingdom Germany France Netherlands Greece Spain Italy Sweden Denmark Finland Republic of Moldova Pregnancies per 1000 Diet and disease 47 Folates and neural tube defects Adequate intakes of folic acid are important in preventing birth defects such as spina bifida. Folate supplementation prior to and during the early weeks of pregnancy prevents up to 75% of neural tube defects occurring in the developing fetus (128). Further, growing evidence indicates that maternal folic acid may reduce the child’s likelihood of CVD in later life (128). The most vulnerable stages of life are during the early weeks of pregnancy, when a woman may not know she is pregnant. Thus, women’s folate status should always be adequate because many pregnancies are not planned. A supplement of 400 µg folic acid has been shown to reduce the incidence of neural tube defects. Such high levels can be achieved through supplementation or fortification, but with difficulty through an unfortified diet. Possible causal factors in folate deficiency are dietary insufficiency from, for example, a low intake of vegetables and from the low bioavailability of some dietary folates. Within the EU, the prevalence of neural tube defects varies widely between countries. Fig. 1.21 shows that it ranged from about 35 cases per 10 000 in certain parts of the United Kingdom and Ireland to just under 11 in Paris, France in the late 1980s (129). Fig. 1.21. Total reported prevalence of neural tube defects in 14 EUROCAT registries, 1980–1986 Source: adapted from EUROCAT Working Group (129). Fetal programming Fetal programming, or the fetal origins hypothesis, suggests that alterations in fetal nutrition and endocrine status result in developmental adaptations that 0 5 10 15 20 25 30 35 40 Glasgow, United Kingdom Dublin, Ireland Northern Ireland, United Kingdom South Glamorgan, United Kingdom Liverpool, United Kingdom Galway, Ireland Groningen, Netherlands Strasbourg, France Odense, Denmark Hainaut, Belgium Florence, Italy Malta Marseilles, France Paris, France Cases per 10 000 population 48 Food and health in Europe predispose an individual to CVD and metabolic and endocrine disease in later life (92,130). Growing evidence links conditions in the intrauterine environment to the later likelihood of adult chronic diseases such as CVD, type 2 diabetes and hypertension (92,130–134). The relevant factors in fetal life include: • intrauterine growth retardation, which can result in low birth weight • premature delivery of a fetus with normal growth for gestational age • intergenerational factors. Effect of maternal weight The incidence of maternal complications increases with increasing body weight. Several studies (135–137) suggest an increased risk of gestational hypertension, gestational diabetes and/or Caesarean delivery among overweight or obese women (138). In contrast, the fetuses of women whose weight is low before conception and/or inadequate during gestation are at increased risk of growth restriction. There is some evidence that low rates of weight gain may be associated with preterm delivery (139,140). Finally, recent studies suggest that overweight and obese women are less successful at initiating and continuing breastfeeding than women of normal weight (141,142). Low birth weight Low weight at birth (less than 2500 g) is the result of either preterm delivery or intrauterine growth retardation, which can be related to the poor nutritional status of the mother. Fig. 1.22 shows the prevalence of low birth weight in groups of countries across the European Region. Rather surprisingly, of the CCEE, only The former Yugoslav Republic of Macedonia shows a significantly higher prevalence than western European countries. Within the EU, the proportion of low-birth-weight children has remained relatively constant over the past 20 years; only the Nordic countries have seen a fall. In contrast, the prevalence of low birth weight appears to have increased in the NIS. In Armenia, for example, preterm delivery was recorded in 5.6% of live births in 1991 and 6.6% in 1996 (123). Births do not always take place in hospital, however, so country information on the prevalence of low birth weight can be incomplete. Further, differences in reporting and the definition of low birth weight may bias figures from the CCEE. In some countries, infants born weighing less than 1000 g are not included because their risk of dying is so high. As a result, the extent to which the present data reflect the real situation is difficult to determine. The definition and collection of data clearly need to be standardized to improve comparisons between countries. Diet and disease 49 0 2 4 6 8 10 12 14 16 18 20 Belgium (1997) United Kingdom (1997) Germany (1999) Austria (2000) France (1998) Switzerland (1999) Ireland (1998) Luxembourg (1998) Denmark (1996) Finland (2000) Norway (1998) Iceland (2000) Andorra (2000) Sweden (1996) Israel (2000) Turkey (1982) Portugal (1999) Malta (2000) Greece (1995) Italy (1998) Spain (1996) San Marino (1983) Tajikistan (2000) Kazakhstan (2000) Turkmenistan (1997) Kyrgyzstan (2000) Uzbekistan (2000) Armenia (2000) Georgia (2000) Russian Federation (2000) Azerbaijan (2000) Ukraine (2000) Republic of Moldova (2000) Belarus (2000) Slovakia (2000) Hungary (2000) Romania (2000) Bulgaria (2000) Poland (1999) Czech Republic (2000) TFYR Macedonia (2000) Slovenia (2000) Croatia (2000) Albania (1990) Yugoslavia (1999) Latvia (2000) Lithuania (2000) Estonia (2000) Prevalence (%) a The former Yugoslav Republic of Macedonia. a Fig. 1.22. Prevalence of low birth weight (
- <2500 g) across the European Region Source: European health for all database, WHO Regional Office for Europe, 2002. 50 Food and health in Europe The high incidence of low birth weight in babies may be one indication of the nutritional inadequacy of the maternal diet. A study of social variation in birth outcome in the Czech Republic noted that mean birth weight fell between 1989 and 1991 and then rose again. The gap in mean birth weight between the babies of mothers with primary education and those of mothers with university education widened by about 40% from 1989 to 1996. The implications are that the relatively poorer birth outcome for less educated mothers may be linked to their nutritional intake before and during pregnancy and that social differences in birth outcome may have increased in the European Region. Having smaller nutrient reserves not only handicaps small infants but also may compromise development of their immune systems and brains. The greater propensity of low-birth-weight infants to infantile anaemia further handicaps cognitive development because of the effects of marked iron deficiency with anaemia on the iron-dependent process of brain development in infancy. Intergenerational factors As mentioned above, young girls who grow poorly become stunted women. They are more likely to give birth to low-birth-weight babies, who are in turn likely to continue the cycle by being stunted in adulthood, and so on. Low maternal birth weight is associated with higher blood pressure levels in a child, independent of the relation between the child’s own birth weight and blood pressure. There are clear intergenerational factors in obesity, such as parental obesity, maternal gestational diabetes and maternal birth weight. Feeding of infants and young children Breastfeeding is the most beneficial way of feeding an infant, as breast-milk provides not only the appropriate amounts of nutrients but a range of other factors that contribute to growth and the development of the immune system and intestines and other organs. For example, the iron in breast-milk is highly bioavailable and is normally sufficient for the needs of a fully breastfed infant up to 6 months of age (http://www.who.int/child-adolescent-health/ NUTRITION/global_strategy.htm, accessed 25 September 2003) (26). Breastfeeding practice varies remarkably between European countries. As Fig. 1.23 shows, at 3 months, over 90% of infants in Uzbekistan are at least partially breastfed, compared with about 25% in the United Kingdom (143). Nevertheless, breastfeeding rates seem to be increasing across the Region. Nordic countries especially have very high rates compared with those 20 years ago. In Norway, for instance, the prevalence of breastfeeding at 3 months rose from only 25–30% in 1969 to about 80% in 1985 (144). Bottle-feeding with Diet and disease 51 10 20 30 40 50 60 70 80 90 100 Azerbaijan (1996) Kyrgyzstan (1997) Uzbekistan (1997) Sweden (1993) Bosnia and Herzegovina (1993) Kazakhstan (1995) Tajikistan (1996) Yugoslavia (1996) Norway (1991) Bulgaria (1989–1996) Republic of Moldova (1996) Poland (1997) Czech Republic (1991) Denmark (1992) Germany (1996) Georgia (1998) Armenia (1993) Ukraine (1996) Estonia (1996) Netherlands (1996) Switzerland (1994) Belarus (1993) Russian Federation (1996) Lithuania (1993) Ireland (1992) Slovakia (1990) Croatia (1995) Luxembourg (1994) Latvia (1996) United Kingdom (1995) 3 months Partial breastfeeding (%) 6 months Fig. 1.23. Percentage of infants being partially breastfed at 3 and 6 months, European Region, 1990s Source: Comparative analysis of implementation of the Innocenti Declaration in WHO European Member States (143). 52 Food and health in Europe cow’s milk, however, is still common throughout the Region, leading to possible gastrointestinal blood loss, micronutrient deficiency and anaemia (27). For example, a survey in Uzbekistan found that 35% of children under 3 months of age were fed using a bottle, 12% with infant formula and 23% with evaporated milk (109). The exclusive breastfeeding of infants is essential for proper growth and development. The weight of current evidence indicates that breastfeeding helps reduce the risk of developing CVD in later life. HIV and breastfeeding About one third to one half of overall mother-to-child transmission of HIV occurs during the period of breastfeeding (145). This overall rate is roughly twice as high in populations where breastfeeding is the norm as in those where it is uncommon (146,147). Several studies have shown that the rate of transmission can be further increased if HIV-positive mothers combine breastfeeding regimes with formula feeding (148,149). The reason may be that feeding with formula introduces foreign bacteria into the infant’s intestinal tract, which alters the mucosal lining’s functioning and its ability to act as a barrier against ingested HIV (150). Clinical risk factors, such as bleeding nipples, mastitis and breast abscesses (151–153), have been associated with mother-to-child transmission of HIV, as has the viral load of the breast-milk. Despite the declining trends in HIV/AIDS in the European Region, HIV continues to spread among injecting drug users in the CCEE and central Asian republics. Until the mid-1990s, this part of the Region appeared to have been spared the worst of the epidemic. It now holds an estimated 270 000 people living with HIV, and AIDS incidence is expected to increase in the near future (http://www.euro.who.int/eprise/main/WHO/Progs/SHA/ Home, accessed 25 September 2003) (see Chapter 4, pp. 244–245, for WHO recommendations). Complementary feeding After 6 months of exclusive breastfeeding, infants should receive other appropriate foods (see Chapter 4, pp. 245–248). As shown in Fig. 1.24, however, this does not always happen in the Region; infants are given water (boiled or not), tea with sugar and cereals as early as 2 weeks in most central Asian republics (80,82,108,109,154–162). These feeding practices can lead to diarrhoeal diseases (Fig. 1.25) and anaemia in both infants and young children (see above) (80–82,108, 109). Growth retardation Poor feeding practices can be considered a major cause of undernutrition. The main manifestation of undernutrition in the Region is stunting: chronic reduc->
Recent Posts
- Tips & Picks from FM Gluten-Free Food Blogger, Cassie Temple from @MyStomachHatesMe
- Upside Foods announces cultivated ground chicken as its second product
- My Turn: Toting up food value of plants vs. animals on a farm
- A search for the best South Jersey spots to dig into plant-based foods
- Oggs Is Making Chicken Eggs Obsolete With More Than 5 Million Sold In 4 Years
Most Used Categories
Trendy Blog - Modern WordPress Theme. All Rights Reserved. Blaze Themes.
Back to top
We use cookies on our website to give you the most relevant experience by remembering your preferences and repeat visits. By clicking “Accept All”, you consent to the use of ALL the cookies. However, you may visit "Cookie Settings" to provide a controlled consent.
Manage consent
Privacy Overview
This website uses cookies to improve your experience while you navigate through the website. Out of these, the cookies that are categorized as necessary are stored on your browser as they are essential for the working of basic functionalities of the website. We also use third-party cookies that help us analyze and understand how you use this website. These cookies will be stored in your browser only with your consent. You also have the option to opt-out of these cookies. But opting out of some of these cookies may affect your browsing experience.
Necessary cookies are absolutely essential for the website to function properly. These cookies ensure basic functionalities and security features of the website, anonymously.
| Cookie | Duration | Description |
|---|---|---|
| cookielawinfo-checkbox-analytics | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Analytics". |
| cookielawinfo-checkbox-functional | 11 months | The cookie is set by GDPR cookie consent to record the user consent for the cookies in the category "Functional". |
| cookielawinfo-checkbox-necessary | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookies is used to store the user consent for the cookies in the category "Necessary". |
| cookielawinfo-checkbox-others | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Other. |
| cookielawinfo-checkbox-performance | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Performance". |
| viewed_cookie_policy | 11 months | The cookie is set by the GDPR Cookie Consent plugin and is used to store whether or not user has consented to the use of cookies. It does not store any personal data. |
Functional cookies help to perform certain functionalities like sharing the content of the website on social media platforms, collect feedbacks, and other third-party features.
Performance cookies are used to understand and analyze the key performance indexes of the website which helps in delivering a better user experience for the visitors.
Analytical cookies are used to understand how visitors interact with the website. These cookies help provide information on metrics the number of visitors, bounce rate, traffic source, etc.
Advertisement cookies are used to provide visitors with relevant ads and marketing campaigns. These cookies track visitors across websites and collect information to provide customized ads.
Other uncategorized cookies are those that are being analyzed and have not been classified into a category as yet.

































































































































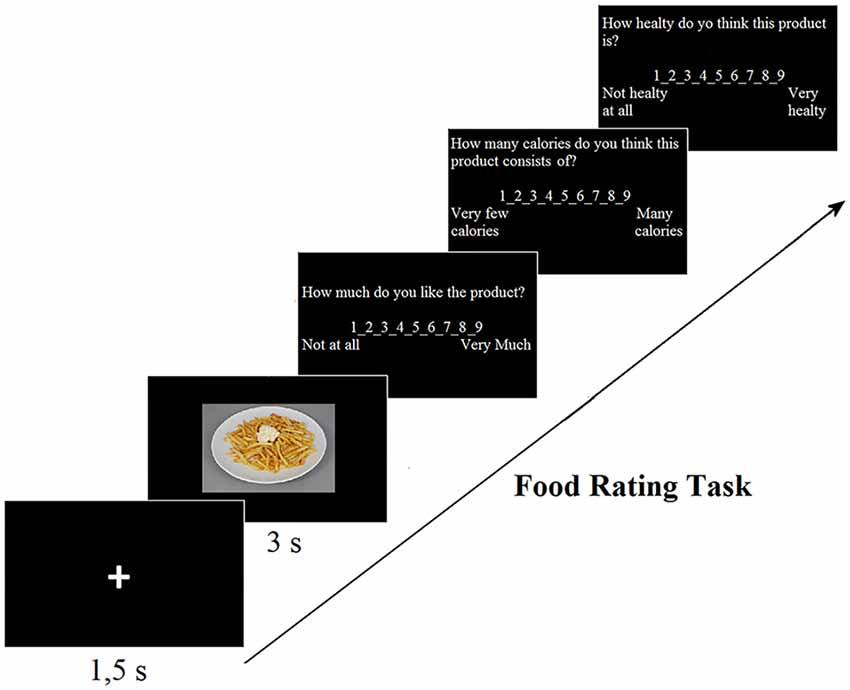





0